Enhancing the value of clinical networks for rare diseases
Abstract
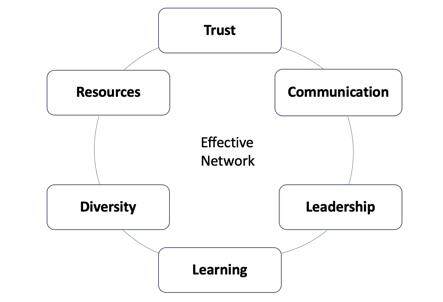
Healthcare networks for rare diseases are developing around the world, concentrating expertise and knowledge from China and Japan to the United States and across Europe. Networked care is scaling up as an effective model of care for rare diseases, with prevention, diagnosis, care and treatment administered locally, informed by the body of knowledge and expertise from the whole network. Now, as the United Nations encourages the development of rare disease networks in all countries, it is timely to reflect on the key characteristics of an effective network. This article aims to identify the core themes needed for a clinical network to be healthy. This article drawing on experience from existing networks through a series of semi-structured interviews, insights from leaders of existing networks are then triangulated with the published evidence. The review aims to identify the themes that allow a clinical network to be effective and flourish. Healthcare networks are best understood as learning systems to generate collaborative knowledge used to inform the best possible care. Six themes are consistently reported in the literature and leaders’ experience: Trust, Communication, Leadership, Learning, Diversity and Resources. Learning together is a key element of the success of effective networks and is most effective when networks are professionally multi-cultural and diverse, including the voices of people living with a rare disease. Patient representative involvement is fundamental to network collaboration and is recognized as a key aspect of early successes. Clinical leadership is critical to providing legitimacy and trust, creating a common identity and promoting collaboration. Networks take time, resources and coordination to develop. Although in-kind support and voluntary contributions of network members are important, inadequate resourcing is a critical barrier to the long-term sustainability and effectiveness of networks. This review explores the core themes of effective networks. Through harnessing digital solutions that enable experts to coordinate care virtually across a clinical network, healthcare for people living with a rare disease is evolving to meet their complex needs. However, payment models to finance these models of care still lag behind innovative healthcare delivery models.
Keywords
INTRODUCTION
In the field of rare diseases, healthcare networks have been born out of necessity to build a critical mass of knowledge and to stimulate new learning. The body of evidence and knowledge related to a specific disease or condition is typically directly proportionate to the size of the affected population. The lower the number of cases, the more limited the opportunity to conduct research and build an evidence base, which in turn disproportionately and adversely influences the quality of life and health outcomes for people living with a rare disease (PLWRD).
The unique features of each rare disease, the majority of which are characterized by high levels of severity and complexity involving multiple organ systems, have pushed traditional models of care. While people with more common diseases are typically treated by a single individual or team within one hospital, PLWRD require a higher degree of coordinated care that goes beyond the delivery of care model based on “multidisciplinary teams”; they require integrated, “networked” care[1]. In such a model, experts are located in multiple healthcare organizations, and highly specialized teams may be based in several different countries. Therefore, technologies are needed to enable clinical teams to effectively collaborate and share the latest knowledge, experience and evidence. These exchanges help inform coordinated care locally for the benefit of all. What was observed during the research is the formalization of casual professional networking complementary and strengthening local healthcare systems.
Healthcare and research networks have taken seed in many health systems, such as the National Collaborative Network for Rare Diseases in China[2], European Reference Networks in the European Union[3,4], Filières Santé Maladies Rares in France, Initiative on Rare and Undiagnosed Diseases (IRUD) Network in Japan[5], Newborn Screening Network in the Philippines, the Undiagnosed Disease Network in the United States[6-9], Undiagnosed Disease Network International[10-14] and the International Rare Disease Research Consortium[15]. Such networks are spreading worldwide as the preferred approach, particularly where affected individuals, experts and knowledge are scarce, as is the case for rare and undiagnosed diseases.
The newly adopted United Nations resolution addressing the challenges of persons living with a rare disease and their families (2021) specifically encourages the creation of networks and the strengthening of international collaboration in the field of rare and undiagnosed diseases. It is, therefore, timely to reflect on the characteristics conducive to a healthy network and the characteristics required to help networks flourish.
This article aims to identify the core themes needed for a clinical network to be healthy, not including the level of funding, quality and sizes of networks. The core themes identified can be used to inform the development and scaling up of new networks and connect existing healthcare networks for rare diseases around the world. This article aims to provide evidence to help inform the development of wide-reaching networks to support people with rare diseases and underpin a structure for: (a) access to care; (b) improving the care they receive; (c) learning from collective experience; and (d) innovating to transform patient health outcomes.
METHODS
The literature on interprofessional collaboration is difficult to retrieve as there are no keywords both sensitive and specific to this subject[16]. Consequently, this review took a pragmatic approach. The search completed on PubMed was limited to literature reviews that included the following terms: “Communities of practice”; “Collaboration”; “Knowledge management”; “Teamwork”; and “Networked”.
In total, 1265 papers were retrieved. Further searches conducted for evidence related to centralization in the context of health networks yielded 225 additional papers. From the 1490 articles retrieved, findings from 65 were included in this synthesis. Taken together, the literature reviews included in this study encompassed within their analyses 1506 primary studies containing a realistic analysis of evidence. Specifically, the studies queried what works for whom, under what circumstances, in what respects, and how[17].
In addition, a series of in-depth interviews were conducted with representatives of key stakeholder groups and partners to discuss their involvement in existing networks and capture their insights into the added value of the networks. The interviews were semi-structured, using a core interview questionnaire, and were conducted via videoconference. The interview questionnaire was structured around three domain areas: (i) Characteristics (Mandate, Structure and Funding); (ii) Content (Model, Scope and Function); and (iii) Added Value (Improvements, Outcomes, Impact and Success Factors).
The interviews focused on ten existing networks, which were identified and selected by engaging leaders from the rare disease community. Three people were interviewed from each selected network, consisting of a clinical lead, patient lead and institutional lead. This method enabled the triangulation of insights and feedback for each of the regional and international networks. A narrative review and a realistic approach synthesis were extracted from the findings of the semi-structured interviews among the different stakeholders, triangulated around each selected network. The findings were organized around the identification of the characteristics and contents of each of the existing networks and mapping of the perceptions of the added value, benefits and impact of each respective approach.
RESULTS
Healthcare networks can be conceptualized as inter-organizational communities that are vehicles for collaborative knowledge management aiming to deliver, and improve upon, the best possible care. When conceptualized this way, the literature provides a substantial amount of information for understanding what the likely facilitators and barriers are to an effective global network for rare diseases.
When creating, developing, or improving healthcare networks, specific themes must be nurtured.
Trust
First, healthcare networks are about connecting people, developing relationships and creating community. It is not surprising, therefore, that the most important and impactful attitude and behavior of an effective network is trust.
Trust is a theme repeatedly linked to the effectiveness of collaborations[18-23]. Furthermore, trust cannot be unilateral; it needs to be mutual[24] and must create reciprocity[25].
Important attitudinal sub-themes that underpin trust are understanding and valuing. Poor understanding across agencies[26] and a lack of valuing across agencies[27] can quickly create barriers to network collaborations. When professionals sense that their opinions are not valued, they often disengage from involvement[27]. This disengagement is most harmful and difficult to identify when it manifests passively. When actors within a network perform work, either with or for other parts of the network, the quality and the timeliness of the work performed are identified as critical elements in the perception of its value and the continued success of the network collaboration[28].
Concerns over issues of fairness and mistrust of motives are key barriers to the effectiveness of collaborations[29]. Therefore, issues of trust and privacy must be pro-actively identified and addressed[26,29,30].
Attitudes and behaviors that foster trust, especially those that promote mutual understanding among groups, are important[31]. The power of active social interactions in networks should not be underestimated or overlooked[32]. The existence of at least some face-to-face interactions in a network is essential to support social interaction and allow trust to develop.
Existing networks typically organize occasional face-to-face meetings to bring together all members of the networks, along with associated stakeholders. This promotes networking and social interaction, which in turn provides the social “glue” needed to sustain and align the various network members working remotely from each other.
The Undiagnosed Disease Network International (UDNI) was established to bring together geneticists, other experts and centers to formally work together and facilitate robust collaborations across different countries. The success of the UDNI is based upon the collaborative nature of the network, which is secured via the establishment of expectations that are clearly delineated in the membership application phase to share data and pool expertise and infrastructures both inside and outside the network. Face-to-face meetings help to form relationships, build trust and provide the opportunity for members to meet and share experiences and expertise to support the development of best practices.
Similarly, the International Rare Disease Research Consortium (IRDiRC) has created a common ground and pre-competitive space for the free exchange of knowledge and expertise. The organization insists on sharing resources, knowledge and expertise and forming a network of trust. The network requires members to commit to active participation, bringing together key actors and giving increased visibility, recognition and acceptance around the essential nature of collaboration, free from competition among members for IRDRC resources.
Communication
The importance of good, open communication should come as no surprise, as it is fundamental to establishing trust and relationships[18,20,24,33-39]. Poor communication is cited as a barrier to effective networks[26]. What is often overlooked, however, is the necessity for frequent communication[21] to foster social interaction and build group identities.
In many countries, rare disease experts are isolated within their health systems. The establishment of clinical networks connects these experts to each other. Experts and highly specialized teams within one network gained motivation as they recognized that through being part of the network, diagnoses and treatments are improved, and the capacity of the whole system was strengthened by their contributions. There were clear benefits and incentives to being in the network, as there was increased communication among clinicians and information exchanges among healthcare organizations and highly specialized teams.
While communication is key to building relationships and a sense of community within a network, external communication is equally important to foster understanding around the value of the network and the benefits of participating in the network, especially for hospital managers and payers. Without a shared and solid understanding of the complementary benefits of participating in the networks, the contributions and support of participating members may remain on a volunteer basis.
Data sharing within the existing networks, for example, in the ERNs, UDN and UDNI, is a basic requirement to provide a common currency for communication and clinical discussion, enable the exchange of experiences and knowledge and identify new and emerging best practices.
Clinical leadership
Clinical leadership has an important place both informally and formally within effective networks[30]. The leaders of a network act as information and relationship brokers[40]. They must understand social entities both to encourage positive actions and to identify detrimental behavior or practices. Key social entities within networks include professional groupings, pre-existing teams and networks and organizations. The network leadership may serve to broker relationships across these social entities, with awareness of existing boundaries, gaps, influences and interactivity[19,41,42].
The most common leadership approach within networks is “collaborative”[34] and often manifests in “unselfish” leadership[24]. Active collaborative leadership is required[34] and called upon to broaden discussions and leverage the strengths of all the network members[27].
Creating an expert community has been identified as a factor that contributes to a network’s success. Clinical leadership is critical not only to provide legitimacy and trust but also to create a common understanding, common interest, common culture and common values, while fostering collaboration across stakeholder boundaries. For example, each ERN has identified a network coordinator and clinical leads for each of the disease-specific and sub-thematic networks, working groups and task forces. The network coordinators, from across the 24 ERNs, collaborate under the Network Coordinators Group to build common policies and approaches that can be utilized within each of the Networks. The ERNs have adopted a collaborative leadership approach and actively involve patient representatives and clinical leads, from different medical disciplines and countries, in network discussions and activities, building a common identity within the network.
Learning together
Shared learning is an essential element for the success of effective networks[21-24,27,33,37,43,44]. One widely repeated approach to shared learning within networked collaborations is through shared goals[21,22,25,37]. Shared goals are best positioned to support shared learning and the creation of knowledge as a process to develop collaboration and actively build the identity of the network[32].
Actively facilitating the exchange of knowledge across the social boundaries that separate groups within the network[33] is an important role of leaders. Certain specific behaviors have been identified as significant to achieve this. The first involves reflection on actions as a group[29], focusing on learning together. The second consists of activities that create relationships among groups with shared concerns and objectives[31], especially activities that develop new capacities within these groups to work together to find, create, share and exploit relevant knowledge[31].
Networking behavior must be promoted[40] and individuals in a boundary spanning role must stimulate interactive relationships between groups that may not ordinarily interact[40]. The network must specifically mobilize those members who can exert positive external influences to promote connections while minimizing the impact of those who exacerbate divides[40].
A lack of coordination among experts threatens network cohesion[27]. Competition among experts can have an even greater impact on the cohesion of the network. Therefore, promoting effective multidisciplinary dynamics is critical to stimulating healthy discussion of complex cases in real time, weighing the risks and benefits of different therapeutic approaches, efficiently communicating treatment plans and mobilizing the required resources[27].
All of the existing networks specializing in rare and undiagnosed diseases have created a common space in which people can share and learn from each other, exchange information on their procedures and develop new tools and approaches. Creating a common space in which to share enables members of a network to broaden their “strategic mindset” into areas that have been underrepresented, e.g., undiagnosed diseases.
Members of the existing networks have reported in the interviews that they benefit from participating in networks from peer learning and professional relationships, as the networks pull together people with similar mindsets, personal commitments and shared interests, strengthening existing networks under one common identity. Members benefit from increased access to a greater pool of expertise and experience and through translating research, innovation and emerging best practices into clinical practice. Case discussion plays a significant role for members to aggregate knowledge and exchange experiences as part of the virtuous cycle of learning. Among the major advantages, what is perceived by network members is the opportunity within the network to provide and obtain feedback on rare and complex cases and to access educational components, such as webinars, conferences and e-learning.
The UDNI was founded on the principles of the well-established Undiagnosed Diseases Network (UDN) in the USA, which works through sharing cases and information. Cases referred to the UDN and subsequently diagnosed are typically a new unknown condition, an existing known disease or a phenotypic expansion. The UDNI was established to connect and foster collaboration among international experts, stimulate the development of undiagnosed disease programs around the world, collaborate on second cases and share cases (and data) through the PhenomeCentral database[45] to help centers identify individuals affected by the same disorder.
The European Reference Networks (ERNs) structure is recognized for its excellence in networking, collaboration and knowledge sharing. Feedback from participants reflects on its lack of adequate support for clinical activities, such as the provision of virtual consultations or expert panels. The ERNs structure provides a system to promote the best clinical care through the development of knowledge to improve diagnosis and therapies, utilizing virtual tools to collaborate and provide guidance to local healthcare services.
The initiative on Rare and Undiagnosed Diseases (IRUD) in Japan combines expertise and technology to develop a systematic approach to supporting patients with medically unidentified conditions and is funded by the Japan Agency for Medical Research and Development. These efforts have led to the construction of a nationwide medical research consortium dedicated to helping patients receive diagnoses. The network enables primary healthcare clinics to collaborate through a learning network of more than 450 hospitals including 37 IRUD Clinical Centres, where complex cases can be reviewed by multidisciplinary IRUD Diagnosis Committees made up of medical specialists and clinical geneticists. As of March 2021, the six-year IRUD project has analyzed 5136 families and confirmed the diagnosis in 2247 (43.7% diagnosis rate by genetic analysis). In addition, 42 new diseases were discovered, of which 13 have already been registered in Orphanet.
Irrespective of the coverage or scope, learning must be at the heart of a network. Experience shared among the members helps to foster sustainable clinical practice and standards across the network and safeguards against individual clinical sites falling behind. For example, the Newborn Screening Network in the Philippines continues to grow and sustain the interest of healthcare professionals by fostering their professional development through medical education and training activities offered through the network, such as attending regular conferences and skills training. The network supports a more integrated approach among screening facilities, diagnostic centers, laboratories and clinics.
Professional multi-cultural and diversity of membership
Network development works most effectively when networks are multi-cultural and culturally safe and responsive. The expertise and experience of the cultural context in which the network will support or deliver care are of great importance, particularly to the “nodes” of the network.
The value of local cultural expertise is a specific example of a more general principle: If the actors in a network are all the same, the network typically cannot and will not flourish. There are various potential reasons for this. Differences in experience lead to mutual giving and gaining of valuable learning[46]; a multi-cultural network provides new channels of information and insight to be accessed, stimulating learning within the network. Networks can have three types of interpersonal connections: strong, weak and invisible. Strong connections are formed by people who operate in the same area or circles and have a lot in common. Weak connections create new routes for information and communication to enter the network. Invisible connections are relationships on the periphery. Paradoxically, the “weak connections” are the most important to the learning of networks[47].
Professional diversity among the membership and their experience is also critical to the success of existing rare disease networks such as the ERNs, UDNI and IRDiRC. At a minimum, membership should include clinicians, researchers and patient representatives. The IRDiRC also successfully brings together payers and industry partners within the network. Patient representative involvement, in particular, is recognized as fundamental to network collaboration and is viewed as a key aspect of early successes.
Networks provide a platform to raise awareness for previously neglected public health priorities and activities. Networks create a space for more integrated action, eliminating isolated activities. Networks enable a community to form with shared experiences, shared problems, shared expertise and shared areas of interest. Prior to the development of networks, each organization typically operated alone, without the possibility to share either their successes or their limitations.
Investment and resources
Inadequate resourcing is a critical barrier to the long-term sustainability and effectiveness of networks[26]. While the projected eventual savings from the integration of networks are anticipated, the real current costs cannot be avoided if success is to be achieved[48]. Asking professionals and managers to cooperate does create costs, which are necessary to coordinate, support and expand their knowledge, perspectives and interests[48].
A key characteristic of effective networks is that they require time. Networks must facilitate processes for social interaction since this is key to knowledge exchange. This process takes time[25,49-52]. A lack of resources to coordinate and facilitate exchanges between members can reduce collaboration within the network, leading members to disengage and potentially causing the downfall of the network.
Investment in networks normally occurs through providing people rather than direct operational funding. While voluntary contributions by network members are a founding principle of clinical and research networks, with members gaining experience, status and personal growth through their participation, this alone does not guarantee that a network will flourish.
At a national level, clinical networks, such as the Newborn Screening Network in the Philippines, are funded through public insurance. The advantage of securing funding as part of the national system allocation is that the underpinning clinical services are given a specific mandate within the healthcare system, allowing for full integration of care across service pathways. All members of China’s National Rare Diseases Collaborative Network are public hospitals under the jurisdiction of the National Health Commission (NHC) and hence must follow the NHC’s mandate. Although members receive no additional funding from the NHC for being part of the network, they benefit by receiving continued medical training from the network (funded through other mechanisms) and being in the center of China’s rare disease expert communities. The network brings direct benefits to PLWRD and their families as it is now much easier to locate rare diseases resources and experts in China, and, once in the network, PLWRD have a greater chance of being referred to the right experts within the network.
For networks that span different countries and regions, anchor grants can be given to support networking, coordination and the digital infrastructure. However, for care provided by a network member in another country, a sticking point is the means by which should be funded. The ERNs are funded through a combination of in-kind contributions of the members, grants from the European Commission, and, for some countries, the coordinating centers receive support from their national authority. The ERNs can also apply for further funding opportunities, such as research grants and activity-specific initiatives for clinical exchange programs and research projects.
In contrast, members of the UDNI and IRDiRC are self-funded for their attendance at network meetings and conferences and participation in jointly funded projects. The IRDiRC also requires member institutions and organizations to provide evidence of a commitment to invest at least 10 million US dollars every five years for rare disease research.
DISCUSSION
Each of the themes highlighted in the study, alone and in isolation, is unlikely to support a network becoming effective. Only together can these core themes create more than the sum of their parts. Clinical leadership builds trust, legitimacy and shared identity through embedding a collaborative spirit between a diverse membership and creating a learning environment for knowledge generation and sharing. Without the necessary resources, time, tools and funding, the ambition of a network will be limited; the collective capacities of the network will fall short of what is needed to allow for the coordination and facilitation of networking activities.
Over the past decade, we have witnessed how to read: the witnessed how the complex needs of people living with a rare disease to realize health equityhave stimulated a paradigm shift in the way highly specialized healthcare can be organized in networked care models. In parallel, digital technologies have matured, providing the opportunity for the isolated and scattered patient population to access expert clinicians for their disease through the establishment of clinical networks that enable the expertise to travel, rather than the person, and inform care locally. Globally, healthcare systems are gaining experience in establishing and delivering clinical networks.
Prior to the COVID-19 pandemic, virtual care was an exception, residing on the margins of healthcare systems. Now, it has become a key part of the “new normal” and a critical part of the rare disease healthcare delivery model that can increasingly be combined with local services. However, whilst virtual care is growing in popularity and use, it does have its limitations and is not a “cure for all”. For example, frontline services for remote regions or for indigenous care will always remain critical to providing equitable access to essential services. The opportunity is ripe for clinical networks for rare diseases to extend throughout all healthcare systems around the world and connect nationally and across regions to allow a global network for rare diseases to take root in all countries.
Virtual consultation and expert panels are established in many existing networks to coordinate advice among professionals. Funding for the clinical work and specialist advice provided through these networks has become a source of tension. How, for example, should experts active in a clinical network be appropriately reimbursed for providing advice and expertise overseas or to a center in another country? The time required for uploading data and managing virtual multidisciplinary team discussions also needs to be acknowledged and compensated.
Since models of care and digital technologies have evolved and demonstrated proof-of-concept, clinical networks now need to be adopted into mainstream healthcare and become a tangible extension of national healthcare systems. Without funding, clinical networks will not be sustainable, especially if based solely on the principles of voluntary cooperation. Resources are needed to coordinate and finance the clinical services and the infrastructure they provide. There is a pressing need to develop innovative funding models for consultations with rare disease experts.
To take the next step in the evolution of highly specialized healthcare, a strategic focus is now needed on innovative financing models. If we are to consider scaling up and leveraging the existing networks under a global network for rare diseases, thereby fulfilling the ambition of the UN Resolution for Universal Health Coverage and the new UN Resolution on addressing the challenges of people living with a rare disease and their families, consideration of sustainable funding mechanisms is essential, to realize health equity for all and sustainable development.
Innovative financing could be created under a diversified business model, which accounts for the time invested by members, and could attract investment from the commercial sector to allow for multi-stakeholder collaboration. However, the governance arrangements for such collaboration would need to put checks and safeguards in place for all stakeholders to maintain autonomy in clinical decision making.
CONCLUSION
While the model of care and care delivery for highly specialized healthcare, especially in rare diseases, has evolved, there is a current need to support clinical networks and integrate them as an extension of local healthcare systems. Significant experience and evidence exist that can be leveraged to support the establishment of healthy clinical networks for rare diseases. Trust, communication, leadership, learning, diversity and resources are the common characteristics found repeatedly both in the published literature and in the reports from leaders of existing rare diseases networks. However, each of these characteristics cannot in isolation drive the necessary development of a new network or improve an existing one. While each characteristic has its own value, when employed together, they are more effective in unlocking the potential of the expertise, knowledge and capabilities of a network as a whole.
DECLARATIONS
Authors’ contributions
Made substantial contributions to conception and design of the study and performed data analysis and interpretation: Bolz-Johnson M, Kenny T
Provided administrative, technical and material support: Clément L, Gahl W, Padilla C, Nishumura Y, Yang R, Sarfaty L, Hoogerbrugge N, Baynam G
Availability of data and materials
Not applicable.
Financial support and sponsorship
This work was supported by Rare Diseases International.
Conflicts of interest
All authors declared that there are no conflicts of interest.
Ethical approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Copyright
© The Author(s) 2022.
REFERENCES
1. Rath A, Salamon V, Peixoto S, et al. A systematic literature review of evidence-based clinical practice for rare diseases: what are the perceived and real barriers for improving the evidence and how can they be overcome? Trials 2017;18:556.
2. Ren Q, Wang J. Network established to collaborate on diagnosis and treatment of rare diseases in China: a strategic alliance backed by tiered healthcare is the key to the future. Intractable Rare Dis Res 2019;8:78-9.
3. Tumiene B, Graessner H, Mathijssen IM, et al. European Reference Networks: challenges and opportunities. J Community Genet 2021;12:217-29.
4. Vos JR, Giepmans L, Röhl C, Geverink N, Hoogerbrugge N. Boosting care and knowledge about hereditary cancer: european reference network on genetic tumour risk syndromes (ERN GENTURIS). Fam Cancer 2019;18:281-4.
5. Adachi T, Kawamura K, Furusawa Y, et al. Japan’s initiative on rare and undiagnosed diseases (IRUD): towards an end to the diagnostic odyssey. Eur J Hum Genet 2017;25:1025-8.
6. Gahl WA, Wise AL, Ashley EA. The undiagnosed diseases network of the national institutes of health: a national extension. JAMA 2015;314:1797-8.
7. Gahl WA, Mulvihill JJ, Toro C, et al. UDN. The NIH undiagnosed diseases program and network: applications to modern medicine. Mol Genet Metab 2016;117:393-400.
8. Ramoni RB, Mulvihill JJ, Adams DR, et al. Undiagnosed Diseases Network. The undiagnosed diseases network: accelerating discovery about health and disease. Am J Hum Genet 2017;100:185-92.
9. Splinter K, Adams DR, Bacino CA, et al. Undiagnosed Diseases Network. Effect of genetic diagnosis on patients with previously undiagnosed disease. N Engl J Med 2018;379:2131-9.
10. Taruscio D, Groft SC, Cederroth H, et al. Undiagnosed diseases network international (UDNI): white paper for global actions to meet patient needs. Mol Genet Metab 2015;116:223-5.
11. Taruscio D, Baynam G, Cederroth H, et al. The Undiagnosed Diseases Network International: Five years and more! Mol Genet Metab 2020;129:243-54.
12. Gahl WA, Markello TC, Toro C, et al. The National Institutes of Health Undiagnosed Diseases Program: insights into rare diseases. Genet Med 2012;14:51-9.
14. Gahl WA, Boerkoel CF, Boehm M. The NIH undiagnosed diseases program: bonding scientists and clinicians. Dis Model Mech 2012;5:3-5.
15. Dawkins HJS, Draghia-Akli R, Lasko P, et al. International Rare Diseases Research Consortium (IRDiRC). Progress in rare diseases research 2010-2016: an IRDiRC perspective. Clin Transl Sci 2018;11:11-20.
16. Supper I, Catala O, Lustman M, et al. Interprofessional collaboration in primary health care: a review of facilitators and barriers perceived by involved actors. J Public Health (Oxf) 2015;37:716-27.
17. Pawson R, Tilley N. Realistic evaluation. Sage Publications; 1997. Available from: https://psycnet.apa.org/record/1997-36931-000 [Last accessed on 6 Apr 2022].
18. Firn J, Preston N, Walshe C. What are the views of hospital-based generalist palliative care professionals on what facilitates or hinders collaboration with in-patient specialist palliative care teams? Palliat Med 2016;30:240-56.
19. Barnett S, Jones SC, Bennett S, Iverson D, Bonney A. General practice training and virtual communities of practice - a review of the literature. BMC Fam Pract 2012;13:87.
20. Bardet JD, Vo TH, Bedouch P, Allenet B. Physicians and community pharmacists collaboration in primary care: a review of specific models. Res Social Adm Pharm 2015;11:602-22.
21. Bookey-Bassett S, Markle-Reid M, Mckey CA, Akhtar-Danesh N. Understanding interprofessional collaboration in the context of chronic disease management for older adults living in communities: a concept analysis. J Adv Nurs 2017;73:71-84.
22. Laverty H, Meulien P. The innovative medicines initiative -10 years of public-private collaboration. Front Med (Lausanne) 2019;6:275.
23. Lemetti T, Stolt M, Rickard N, Suhonen R. Collaboration between hospital and primary care nurses: a literature review. Int Nurs Rev 2015;62:248-66.
24. Rumping S, Boendermaker L, de Ruyter DJ. Stimulating interdisciplinary collaboration among youth social workers: a scoping review. Health Soc Care Community 2019;27:293-305.
25. Halonen JI, Atkins S, Hakulinen H, Pesonen S, Uitti J. Collaboration between employers and occupational health service providers: a systematic review of key characteristics. BMC Public Health 2017;17:22.
26. Cooper M, Evans Y, Pybis J. Interagency collaboration in children and young people’s mental health: a systematic review of outcomes, facilitating factors and inhibiting factors. Child Care Health Dev 2016;42:325-42.
27. Kabrhel C. Achieving multidisciplinary collaboration for the creation of a pulmonary embolism response team: creating a “Team of Rivals”. Semin Intervent Radiol 2017;34:16-24.
28. Kleijnen S, Toenders W, de Groot F, et al. European collaboration on relative effectiveness assessments: what is needed to be successful? Health Policy 2015;119:569-76.
29. McLoughlin C, Patel KD, O’Callaghan T, Reeves S. The use of virtual communities of practice to improve interprofessional collaboration and education: findings from an integrated review. J Interprof Care 2018;32:136-42.
30. Fung-Kee-Fung M, Watters J, Crossley C, et al. Regional collaborations as a tool for quality improvements in surgery: a systematic review of the literature. Ann Surg 2009;249:565-72.
31. Conklin J, Lusk E, Harris M, Stolee P. Knowledge brokers in a knowledge network: the case of seniors health research transfer network knowledge brokers. Implement Sci 2013;8:7.
32. Li LC, Grimshaw JM, Nielsen C, et al. Use of communities of practice in business and health care sectors: a systematic review. Implement Sci 2009;4:27.
33. McInnes S, Peters K, Bonney A, Halcomb E. An integrative review of facilitators and barriers influencing collaboration and teamwork between general practitioners and nurses working in general practice. J Adv Nurs 2015;71:1973-85.
34. Son D, Kawamura K, Nakashima M, Utsumi M. [The pharmacist-physician collaboration for IPW: from physician’s perspective]. Yakugaku Zasshi 2015;135:109-15.[PMID:25743910 DOI:10.1248/yakushi.14-00222-4] Caution!
35. Eikey EV, Reddy MC, Kuziemsky CE. Examining the role of collaboration in studies of health information technologies in biomedical informatics: A systematic review of 25 years of research. J Biomed Inform 2015;57:263-77.
36. House S, Havens D. Nurses’ and physicians’ perceptions of nurse-physician collaboration: a systematic review. J Nurs Adm 2017;47:165-71.
37. Karam M, Brault I, Van Durme T, Macq J. Comparing interprofessional and interorganizational collaboration in healthcare: a systematic review of the qualitative research. Int J Nurs Stud 2018;79:70-83.
38. Dellinger EP. Teamwork and collaboration for prevention of surgical site infections. Surg Infect (Larchmt) 2016;17:198-202.
39. Havyer RD, Nelson DR, Wingo MT, et al. Addressing the interprofessional collaboration competencies of the association of american medical colleges: a systematic review of assessment instruments in undergraduate medical education. Acad Med 2016;91:865-88.
40. Braithwaite J. Bridging gaps to promote networked care between teams and groups in health delivery systems: a systematic review of non-health literature. BMJ Open 2015;5:e006567.
41. Mulvale G, Embrett M, Razavi SD. ‘Gearing Up’ to improve interprofessional collaboration in primary care: a systematic review and conceptual framework. BMC Fam Pract 2016;17:83.
42. Lunden A, Teräs M, Kvist T, Häggman-Laitila A. A systematic review of factors influencing knowledge management and the nurse leaders’ role. J Nurs Manag 2017;25:407-20.
43. Bollen A, Harrison R, Aslani P, van Haastregt JCM. Factors influencing interprofessional collaboration between community pharmacists and general practitioners-a systematic review. Health Soc Care Community 2019;27:e189-212.
44. Trier H, Valderas JM, Wensing M, Martin HM, Egebart J. Involving patients in patient safety programmes: a scoping review and consensus procedure by the LINNEAUS collaboration on patient safety in primary care. Eur J Gen Pract 2015;21 Suppl:56-61.
45. Buske OJ, Girdea M, Dumitriu S, et al. PhenomeCentral: a portal for phenotypic and genotypic matchmaking of patients with rare genetic diseases. Hum Mutat 2015;36:931-40.
46. Barry M, Kuijer-Siebelink W, Nieuwenhuis L, Scherpbier-de Haan N. Communities of practice: a means to support occupational therapists’ continuing professional development. A literature review. Aust Occup Ther J 2017;64:185-93.
47. Braithwaite J. Between-group behaviour in health care: gaps, edges, boundaries, disconnections, weak ties, spaces and holes. A systematic review. BMC Health Serv Res 2010;10:330.
48. Leutz WN. Five laws for integrating medical and social services: lessons from the United States and the United Kingdom. Milbank Q 1999;77:77-110, iv.
49. Heip T, Van Hecke A, Malfait S, Van Biesen W, Eeckloo K. The effects of interdisciplinary bedside rounds on patient centeredness, quality of care, and team collaboration: a systematic review. J Patient Saf 2022;18:e40-4.
50. Mahdizadeh M, Heydari A, Karimi Moonaghi H. Clinical interdisciplinary collaboration models and frameworks from similarities to differences: a systematic review. Glob J Health Sci 2015;7:170-80.
51. Stolp S, Bottorff JL, Seaton CL, et al. Measurement and evaluation practices of factors that contribute to effective health promotion collaboration functioning: A scoping review. Eval Program Plann 2017;61:38-44.
Cite This Article
Export citation file: BibTeX | RIS
OAE Style
Bolz-Johnson M, Clément L, Gahl W, Padilla C, Nishumura Y, Yang R, Sarfaty L, Hoogerbrugge N, Baynam G, Kenny T. Enhancing the value of clinical networks for rare diseases. Rare Dis Orphan Drugs J 2022;1:9. http://dx.doi.org/10.20517/rdodj.2022.01
AMA Style
Bolz-Johnson M, Clément L, Gahl W, Padilla C, Nishumura Y, Yang R, Sarfaty L, Hoogerbrugge N, Baynam G, Kenny T. Enhancing the value of clinical networks for rare diseases. Rare Disease and Orphan Drugs Journal. 2022; 1(2): 9. http://dx.doi.org/10.20517/rdodj.2022.01
Chicago/Turabian Style
Bolz-Johnson, Matthew, Louise Clément, William Gahl, Carmencita Padilla, Yukiko Nishumura, Rachel Yang, Lisa Sarfaty, Nicoline Hoogerbrugge, Gareth Baynam, Thomas Kenny. 2022. "Enhancing the value of clinical networks for rare diseases" Rare Disease and Orphan Drugs Journal. 1, no.2: 9. http://dx.doi.org/10.20517/rdodj.2022.01
ACS Style
Bolz-Johnson, M.; Clément L.; Gahl W.; Padilla C.; Nishumura Y.; Yang R.; Sarfaty L.; Hoogerbrugge N.; Baynam G.; Kenny T. Enhancing the value of clinical networks for rare diseases. Rare. Dis. Orphan. Drugs. J. 2022, 1, 9. http://dx.doi.org/10.20517/rdodj.2022.01
About This Article
Copyright
Data & Comments
Data
 Cite This Article 17 clicks
Cite This Article 17 clicks













Comments
Comments must be written in English. Spam, offensive content, impersonation, and private information will not be permitted. If any comment is reported and identified as inappropriate content by OAE staff, the comment will be removed without notice. If you have any queries or need any help, please contact us at support@oaepublish.com.