The importance of psychological support for parents and caregivers of children with a rare disease at diagnosis
Abstract
Rare diseases are complex and difficult to diagnose, with parents and caregivers often reporting significant delays in receiving a definitive diagnosis. Following diagnosis, parents and caregivers often feel overwhelmed with emotions, including relief, guilt, and shock. The culmination of this emotional burden may lead to a deterioration of psychological health, ultimately reaching a stage where the parents struggle to cope. A systematic literature review was conducted of the articles on this topic by searching the electronic database, PubMed. Further studies were retrieved from a reference listing of relevant articles and consultation with experts in the field. The review was based on the guidance in the Preferred Reporting Items for Systematic Reviews and Meta-Analyses protocol. The initial search identified 1276 articles, of which 37 met the inclusion criteria and were included in this review. The literature revealed key factors that appeared to contribute to psychological stress, including prolonged diagnostic odyssey, poor diagnostic delivery, lack of information and specialist knowledge, and convoluted healthcare systems. This review reinforces the need for psychological support amongst parents and caregivers of children with a rare disease at the time of diagnosis. The results of this literature review will be used to develop a statement of good practice for the support of parents and caregivers when a rare disease diagnosis is given.
Keywords
INTRODUCTION
A rare disease is characterised as a disease or condition that affects less than 1 in 2000 people within the general population[1]. There are between 6000 to 8000 rare diseases, which affect approximately 29 million people across the European Union[2]. Since each rare disease affects a fraction of the general population, funding for research into causes and potential therapies is scarce[3]. Although each rare disease is distinct, most are complex, degenerative, and life-limiting. Clinical signs and symptoms are variable, difficult to diagnose, and many symptoms overlap with more common disorders, which make diagnosis problematic[4].
As with all life-changing illnesses, it is important for families to obtain answers quickly, minimise the distress of reaching such a diagnosis, and come to terms with their situation[4]. Traditionally, the general practitioner (GP) is the first point of call for concerned families, but due to unfamiliarity with rare diseases, most fail to suspect cases when they present[5]. This leads to referral opportunities being missed, and parents frequently report a delay of several years between first symptom onset and the achievement of a definitive diagnosis[6]. During this time, parents must endure a “diagnostic odyssey”, a term used to describe the multiple referrals and numerous assessments parents face on their journey to a final diagnosis[1,4]. The psychological burden experienced by parents and families during the time taken to reach a diagnosis is followed by the sudden impact and distress felt at the point of a rare disease diagnosis, which can lead to feelings of helplessness and isolation[6].
At the time of diagnosis, parents experience contradicting emotions, often feeling torn between feelings of guilt and/or sorrow and feelings of relief that their wait for answers has come to an end[7]. The consequences of receiving a rare disease diagnosis within the family elicit intense emotions such as anger, shock, anguish, fear, and denial. These feelings are accompanied by the swift realisation that life will never be the same again[8]. The diagnosis marks the start of a new life that parents and caregivers have had little or no preparation for, which may result in a worsening of their own mental and emotional health before adapting to the diagnosis[8].
Currently, no published consensus guidelines exist on the type and extent of psychological support needed by families and caregivers of children affected by a rare disease around the time of diagnosis. Here, we report the evidence collected from a systematic literature review of articles focusing on the psychological impact that actions and interventions have around the time of the diagnosis. These include factors that have a negative impact around the time of diagnosis, such as prolonged diagnostic odyssey, poor diagnostic delivery, lack of information and specialist knowledge, maze-like healthcare systems and forgotten family members. This report focuses on diagnoses of rare diseases made in infancy and early childhood, although the findings and their implications are likely to be more widely applicable. While there are significant psychological sequelae of living with a rare and complex disease, the focus is on the support that could be built around the crucial time of the diagnosis, as this appears to lay the foundations of much of the family experiences, and how they perceive and react to other events in their journey. The results of this review will be used to develop a statement of good practice for the support of parents and caregivers when a rare disease diagnosis is given.
METHODS
The Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines were used to conduct this review[9,10].
Information sources and search strategy
Studies were identified by searching the electronic database, PubMed. To source relevant information, the keywords “psychological support AND rare disease” were used. The search strings incorporated free text key words and Medical Subject Heading (MeSH): (“psychologic”[All Fields] OR “psychological”[All Fields] OR “psychologically”[All Fields] OR “psychologization”[All Fields] OR “psychologized”[All Fields] OR “psychologizing”[All Fields]) AND (“support”[All Fields] OR “support s”[All Fields] OR “supported”[All Fields] OR “supporter”[All Fields] OR “supporter s”[All Fields] OR “supporters”[All Fields] OR “supporting”[All Fields] OR “supportive”[All Fields] OR “supportiveness”[All Fields] OR “supports”[All Fields]) AND (“rare diseases”[MeSH Terms] OR (“rare”[All Fields] AND “diseases”[All Fields]) OR “rare diseases”[All Fields] OR (“rare”[All Fields] AND “disease”[All Fields]) OR “rare disease”[All Fields]). Further studies were retrieved from consultation with experts in the field and reference listings of relevant articles. The expert group consisted of clinicians with expertise in psychology, paediatrics, genetics, experts in the delivery of mental health support in rare diseases, professional counsellors, parents of children with a rare disease, and a person with a rare disease.
Inclusion criteria
Study design
Studies that included the psychological impact on parents and caregivers at the time of diagnosis of a rare disease were considered for inclusion. We did not exclude any study design, nor were there exclusions based on sample size, length of follow-up, or country. Letters to the editor, and book chapters were excluded.
Study selection and data extraction
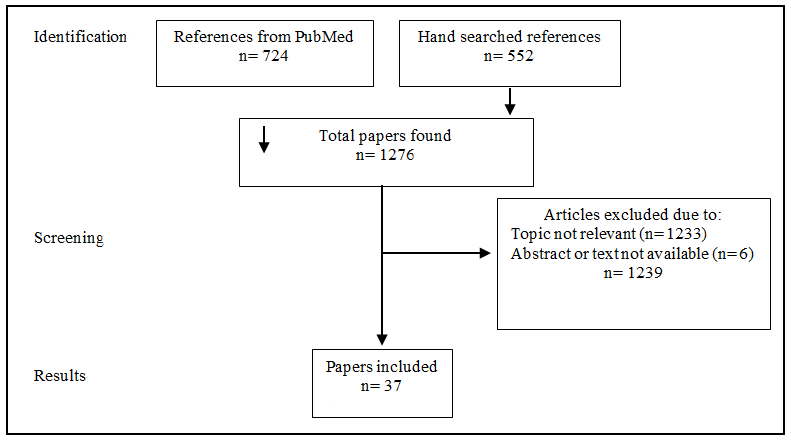
All references identified through the search strategy were downloaded into Endnote Version X9. Two reviewers independently screened the references for potential inclusion based on title and abstract. Reviewers were not blinded to the study author or journal. A third reviewer was planned to be used to mediate any disagreements until consensus was reached; however, this was not required. Several study authors were contacted directly for full-text articles, and one author was contacted to provide clarification on study methods. The full texts of studies deemed potentially eligible for inclusion were obtained, and two reviewers independently assessed them for eligibility. Those studies deemed as ineligible were recorded with reasons for ineligibility. A flow chart [Figure 1] was created, following the PRISMA protocol to illustrate this process[10]. A total of 1276 papers were identified and screened. Of these papers, 1239 were excluded due to irrelevance or unavailability of the text, and the remaining 37 papers were taken forward for inclusion in this review[1,2,4,6-8,11-41]. The reviewers independently extracted data onto a piloted data extraction form developed for this review, with discrepancies resolved via consensus discussion.
RESULTS
Of the 37 papers included for review, only two contained quantitative data, with the remaining comprising qualitative data. A wide range of rare diseases was explored, including lysosomal storage diseases and mitochondrial diseases. Study details and key findings are presented in Supplementary Table S1. In most studies, response rates from participants were high, and several studies were the first of their kind focusing on that disease. Study limitations included small sample sizes, which were not always representative of the rare disease population, for example, some studies recruited respondents from one hospital and in other studies, fathers were vastly underrepresented.
Prolonged diagnostic odyssey
Rare diseases are complex and challenging to diagnose; families of affected children often have to wait years from first symptom onset to receive a final diagnosis[1,4]. This delay in diagnosis causes strong feelings of confusion, despair and uncertainty, which appear to intensify the longer the pre-diagnostic period lasts[35]. Parents will often feel a sense of loss for the life they were used to before the disease and may yearn for what they perceive as a normal family life[6]. For most parents, the time from the onset of first symptoms to final diagnosis is the most challenging and psychologically tough[6,35].
During the process of seeking a diagnosis, affected children may face a deluge of assessments and examinations, which causes great emotional strain on the family. Parents frequently consult multiple doctors and health specialists regarding their child’s symptoms, often receiving several incorrect diagnoses before the correct diagnosis is received[2]. This long, convoluted path to diagnosis can be a considerable source of stress and anxiety for parents, of which the short-term and long-term psychosocial effects remain unknown[40]. A recent study found that ~35%-40% of parents with undiagnosed children met the criteria for mild to moderate anxiety and depression[40]. Another study demonstrated high levels of anxiety and stress in parents caring for children with a rare disease, associated with an apparent lack of knowledge among health professionals and unavailable or delayed testing[1,24].
Upon receiving a definitive diagnosis of a rare disease, parents may experience overwhelming feelings of shock and relief[7]. A conclusive diagnosis gives parents a sense of control, allowing parents to become more accepting of the situation and better able to care for the needs of the child through agreed treatment/management plans[22]. Although parents may feel initial relief at finally reaching a diagnosis, some parents also experience a loss of hope, feelings of guilt, and often become disconnected from their social network of peers[20].
Poor diagnostic delivery
The manner in which a diagnosis is delivered has a substantial effect on the family’s immediate and long-term psychological and emotional wellbeing. Parents more able to cope with the diagnosis will positively influence how their affected child will adjust to the disease[6]. A constructive experience at this critical time can leave parents feeling well-informed, supported, and able to plan for the future[4]. A negative experience can lead to parents “falling apart” or even concealing the diagnosis[41].
A successful diagnosis delivery is centred around three key factors: time, information, and compassion[1]. Healthcare professionals must allow enough time to clearly explain the nature of the disease, effects on daily life, disease progression, and prognosis. Parents and families need to be in a comfortable environment and feel able to ask any questions they may have[2]. Immediately after receiving the diagnosis, parents should be signposted to patient organisations that can offer psychosocial support and also provide them with contact details for parental support groups[16]. Post-diagnosis check-ins by trained healthcare professionals should be made available in the months following diagnosis[18].
The most common issues cited among families that had a negative experience included a lack of empathy, lack of information about the condition, and avoidable delays[4,22]. Parents thought there was a significant lack of awareness amongst healthcare professionals, adding that some did not seem to appreciate how devastating the diagnosis was[4,31]. In one case, the paediatrician walked out half-way through delivering the diagnosis[1].
In addition to insensitive communication and inadequate information, parents also identified an absence of psychological support at the time of diagnosis[1]. Some parents were completely alone when they received the diagnosis of a rare life-limiting condition for their child, and a recent study found that most families received the diagnosis over the telephone rather than face-to-face in the clinic[1,4,32]. The stress and trauma caused during this time may cause severe deterioration in mental health, with some parents experiencing potential trauma[35].
Lack of information provision
Following diagnosis, parents often felt overwhelmed, scared, and isolated, with little support and information from health care providers[17,22]. Parents and families were left frustrated and perplexed by the absence of knowledge and signposting to relevant support services and information[17]. This was compounded by the apparently extensive information that is readily available and provided for other childhood illnesses[22]. A lack of information added to the uncertainty experienced by parents and impeded their ability to manage and cope with their child’s condition. However, through education, parents were better able to cope with stressful situations[8,11].
Some parents reported that health care providers withhold information deliberately, perhaps to shield the family from undue distress or possibly because they deemed the information too complicated for the layperson. This led to further feelings of isolation and the inability to trust and rely on healthcare providers for information and guidance[17]. Healthcare professionals must adapt their communication style to share their knowledge in a way that parents are able to understand, by simplifying medical terminology and taking time to explain complexities[7]. The availability of take-away, written materials is essential to ensure that information relayed in the clinic is not forgotten.
Due to the lack of available information, parents are often left to their own devices to answer their own questions. To combat uncertainty, parents will gather as much information as possible through patient organisations, social media, and searching the internet[20]. However, there are drawbacks to researching information online; many parents find accessing meaningful and accurate information is difficult. Information from unmanaged sources, including social media, often triggers chronic sorrow, fear, and anxiety through negative information and information overload[8,17]. Parents’ support groups fulfill a precious function of peer support, where parents are able to establish relationships with others going through a similar experience[17,38]. Online support groups provide a space for meeting and interacting with other careers, although some felt that the online community could not replace face-to-face interactions[17].
Parents wanted information on their child’s prognosis, management of care, and the impact of prescribed medicines on development. Without this information, parents felt that it hindered their ability to cope when situations arose. In addition, parents wanted specific information on long-term services, financial assistance and support available in the community, so they were able to make plans for the future[8]. Parents also expressed interest in educational resources that they could pass on to friends and family to clearly explain their child’s disease[8].
Lack of specialist knowledge
A significant cause of stress and exasperation experienced by parents of children with a rare disease is the seemingly profound lack of knowledge and awareness amongst healthcare professionals[2]. This may be due to a number of factors, such as the rarity of the disease, the absence of available testing, and inadequate training during medical studies[1]. Many existing information resources appear to be overlooked by healthcare professionals, including resources to support clinical care, clinical guidelines on diagnosis and treatment, and directories of specialised clinics and referral pathways[1]. This lack of specialist knowledge has grave implications, including a delay in diagnosis, which may prevent or alter the treatment that the child is able to receive[1]. In some instances, the absence of information meant that parents felt the need to source material themselves, despite the difficulty in obtaining accurate information without guidance[24].
Parents may feel rejected by healthcare professionals due to their limited understanding of the obstacles encountered by children with rare diseases, which are significantly different from those not living with them[2,12,24]. However, the knowledge required by parents of an affected child is far more substantial than that normally demanded by parents to adequately care for their child. Parents must increase their health literacy, specialist health knowledge, and develop their caregiving skills to effectively parent a child with a rare disease[24]. Parents reported the anguish of not being believed by the GP and, subsequently, their child not being referred to a specialist[2,22]. In some cases, patients have been referred to another specialist equally unfamiliar with the disease, passing the responsibility onto someone else[2].
Misdiagnosis is common, particularly incorrect psychiatric diagnoses, which causes great frustration and mistrust[2]. Even when a rare disease is correctly diagnosed, parents may seek the reassurance of a second opinion, which can sometimes lead to a breakdown in the relationship with the first doctor[2]. In addition, parents may begin to lose hope in the conventional healthcare system, leading them to turn to alternative medicine to receive acknowledgement and support[2].
Unassessed psychological need
Many parents are fearful of the long-term implications of a rare disease, which inevitably has an effect on the entire family[13]. The psychosocial impact was found to be particularly significant at the time of diagnosis of a rare disease, notably in families of children with genetic metabolic diseases who have had to wait a long time for a definitive diagnosis[1]. Few families appear to be offered psychological support or counseling at the time of diagnosis, and many have no access to peer support groups[1,4]. If offered, most parents preferred face-to-face professional support, although a combination of in-person and online sessions was more viable. Group sessions also added opportunities to build wider support networks and facilitated the sharing of experiences with other parents in similar situations[16].
Many parents and families must make tremendous sacrifices and experience social isolation and financial adversity to meet the high level of care required to manage the disease[1,13]. These long-term challenges have a direct impact on psychological health[13]. Peer parent social support or “parent mentors” have been shown to improve parental adjustment to coping with a rare disease diagnosis by offering emotional support, specific information, and a level of compassion that only a parent with shared experiences can offer[18]. A combination of physical, cognitive, and behavioural coping techniques can also be taught to alleviate stress[11].
A French study undertaken to better understand the daily lives of patients and families living with rare diseases found that psychological evaluation and support was highly variable[41]. The study highlighted the social and psychosocial consequences that may develop when faced with a rare disease diagnosis, in particular feelings of isolation and social exclusion[41]. In another study, parents consistently reported elevated levels of depression, anxiety, and stress. The level of stress experienced by parents, in combination with other mental health issues, suggest an enormous demand for psychological support from mental health professionals or peer support groups[1].
Maze-like healthcare systems
Families expressed their frustration and exhaustion towards what they experienced as disjointed and apathetic healthcare systems. Parents of children with rare diseases regularly reported a lack of communication and understanding by healthcare providers, with poor coordination between hospitals[32]. Often, families were forced to manage and coordinate their own healthcare needs by developing their own strategies[6]. The majority of parents would ideally like their GP to coordinate services to meet their child’s healthcare needs[1].
Parents describe the current healthcare system as like a revolving door, in which they repeatedly enter and exit, each time having to tell their story to a different professional[32]. Currently, healthcare professionals with expertise in a given field will provide care for specific elements of the condition, rather than being concerned with the condition as a whole[32]. This can lead to bureaucratic complications when attempting to navigate the social and healthcare systems and to feelings of vulnerability, being lost within the system and falling through the net[6,32].
Ignored practical needs
Parents of children with intellectual disabilities were confronted with a multitude of challenges, which impacted every aspect of their lives, with serious consequences on their work, housing, finances, and relationships[30]. Most parents felt they could not share the burden of care with others, causing huge disruption, strain, and segregation in the family[30].
The substantial emotional burden experienced by parents of children with a rare disease often correlated with poor mental health[36]. This was amplified by disruption to normal life and the personal sacrifices parents must make to manage the disease and adapt to the “new normal”[29]. Parents frequently decided to work fewer hours, switch careers, or take a leave of absence to care for their child[29]. The costs of caring for a child with a rare disease can be substantial. In addition to day-to-day care, families may need to pay for travel costs and for adaptations to the family home to cater for their child’s disability or special needs adaptations[20]. Some parents reported using the internet and social media to access resources and connect with other families going through similar hardships. Support from family, friends and peers was considered vital for family wellbeing[29].
Forgotten family members
The psychological and systemic health of the whole family was impacted by having a child with a rare disease[13]. Mothers of affected children were more likely to suffer from poor mental health and impaired quality of life compared to fathers[13]. Indeed, the parents of an affected child must accept that their own desires may not be met or achieved, and they may experience a lower level of life satisfaction[2]. The mental and emotional toll on parents is also commonly shared by siblings, who experience a complex range of contradictory feelings, including guilt, pride, worry, and sadness[2]. The daily lives of siblings of children with a rare disease can be greatly impacted if family life is centred around caring for their brother or sister, and attention must be paid to supporting their emotional and social needs[2].
DISCUSSION
A thorough review of the existing literature demonstrates the need for family psychological support at pre-diagnosis, diagnosis, and post-diagnosis stages of a rare disease. These results are reinforced by other studies that have examined the supportive care requirements of patients living with rare diseases[42-44]. Studies have shown that early and timely intervention can limit psychological distress and have an encouraging influence on the wellbeing of parents and caregivers[15,45,46]. In many cases, parents and caregivers found the period leading up to diagnosis the most difficult to cope with, and the longer the diagnostic delay, the greater the psychological burden on the family appeared to be. Intervention at diagnosis in the form of psychosocial support and counseling can prevent years of psychological distress for parents[45]. Previous studies have demonstrated improved quality of life outcomes when early psychosocial assessment and monitoring is implemented[47]. There is also evidence that long-term support can improve family members’ wellbeing, help to strengthen relationships and prevent relationships from breaking down[47].
The manner in which a diagnosis is given is vital to patient and family wellbeing moving forwards. A positive experience may be typified by using a validated framework to support the delivery of distressing information. The SPIKES protocol provides a step-wise framework for discussion, with each letter representing a step in the sequence: setting, perception, invitation/information, knowledge, empathy, summarise/strategise[48]. The components of the SPIKES protocol are intended to make the sensitive process of sharing a diagnosis as comfortable as possible for all involved.
Following diagnosis, parents and caregivers take on the responsibility of caring for a child with a rare disease suddenly, with inadequate preparation and support. This is compounded by a wide range of conflicting emotions experienced by the whole family, which may require different degrees, and types, of psychosocial intervention. The development of support systems at this time is vital and can help to alleviate depression by reducing feelings of isolation[49]. Support networks are facilitated by patient organisations that are often able to organise family and scientific conferences. Conference attendance allows families and people with rare diseases to receive up-to-date information and to provide each other with emotional support and companionship[50,51]. Families feel comfortable being surrounded by people in comparable situations, and there is a feeling of normality and solidarity[50]. This is particularly evident for siblings of children with a rare disease, who may struggle to find support from others in a similar position[52].
Our findings highlight key risk factors that contribute to high levels of depression, anxiety, and stress within the parental and caregiving community. These include poor diagnostic delivery, lack of accurate information and a shortage of specialist knowledge available. This study has several limitations, including the challenge of interpreting the literature, as different medical systems may result in a range of experiences of the “diagnostic odyssey” for parents. There will also be a variation in different countries/regions and amongst different cultures in terms of how rare diseases are perceived. This is even more so the case when there is a genetic and an inheritable genetic basis to a condition. Likewise, the palatability of psychological support varies across and between cultures, which really stresses the need for culturally sensitive approaches. This study primarily used PubMed for searching references and given that the aim was to understand the psychological impact on parents and caregivers of children with rare diseases, searching additional databases such as PsycINFO may be beneficial. Additional restrictions such as “at diagnosis” could also be incorporated into the original database searches to narrow the scope of the results.
Some progress has been made in the rare disease arena with the evolution of the European Reference Networks (ERNs) and the Rare Diseases Clinical Research Network in the USA. ERNs allow healthcare workers across Europe to share knowledge on complex cases and rare diseases, enabling the forging of cross-border collaborations. Since leaving the EU, a number of UK providers have been approved to become part of the ERNs[53]. Many ERNs have developed telemedicine strategies for the diagnosis and management of patients, including the Clinical Patient Management System, which offers online, clinical consultations between international experts and clinicians[54]. Another initiative termed: The Global Commission to End Diagnostic Odyssey for Children with a Rare Disease was formed in 2018 to bring multidisciplinary experts in the rare disease and technology communities together. This collaboration led to a series of actionable recommendations with a view to lessen the time taken to diagnose a rare disease[55]. Several telemedicine pilot studies are underway, including the use of a digital tool to provide genetic counselling to patients remotely, and a tool that uses artificial intelligence to support healthcare providers by linking unrelated symptoms to make a rare disease diagnosis[56].
In the UK, highly specialised services are provided to approximately 500 patients per year. The Rare Diseases Advisory Group is responsible for making proposals to the National Health Service (NHS) England and the devolved administrations of the other UK nations (NHS Scotland, NHS Wales, and NHS Northern Ireland)[57]. These recommendations have led to vast improvements in the standard of care patients have received. For example, NHS England commissioned Bardet-Biedl Syndrome (BBS) UK together with specialist centres to provide multidisciplinary clinics to patients with BBS[58]. In one visit to the clinic, patients are seen by a multidisciplinary team comprising a geneticist, clinical psychologist, ophthalmologist, dietician, endocrinologist, speech and language therapist, and nephrologist. BBS UK representatives also offer patients and their families emotional and practical support[58].
The Department of Health and Social Care published the UK Rare Diseases Framework in January 2021[59]. The framework was designed by the governments of all four UK nations with the aim of improving the care and support of the rare disease community. The framework was underpinned by the results of a survey launched in 2019, which sought the views of patients, families, rare disease patient organisations, researchers, and clinicians. The framework identified four key priorities over the next five years: 1) Receiving a final diagnosis sooner; 2) Increasing the awareness of rare diseases amongst healthcare professionals; 3) Better coordination of care; 4) Improving access to specialist care, treatments, and drugs. The action plans for each UK nation are due to be published imminently[59].
Despite significant headway being made within the rare disease field as a whole, rare diseases still lag behind other diseases in terms of published guidelines on psychosocial management. At present, patient organisations are often the only source of trustworthy information and support to newly diagnosed patients and their families[50]. In summary, our review emphasises the unmet need for psychosocial support around the time of diagnosis among the parents and caregivers of children affected by rare diseases.
DECLARATIONS
Acknowledgments
We would like to thank Dr Ella Lineham, Rare Disease Research Partners, for her professional writing services in the preparation of this manuscript.
Authors’ contributions
Substantial contributions to the interpretation of data for the work, revising the draft critically for important intellectual content and final approval of the version to be published: Kenny T, Bogart K, Freedman A, Garthwaite C, Henley S, Bolz-Johnson M, Mohammed S, Walton J, Winter K, and Woodman D.
Availability of data and materials
Not applicable.
Financial support and sponsorship
This work was supported in full by a grant from RBW Consulting (www.rbwconsulting.com) to the Society for Mucopolysaccharide Diseases (Registered Charity No. 1143472. Registered as a Company limited by guarantee in England & Wales No. 7726882. Registered as a Charity in Scotland No. SCO41012). The research was undertaken by the Society for Mucopolysaccharide Diseases’ wholly owned subsidiary, Rare Disease Research Partners. Grant name: Psychological Support for Parents and Caregivers of Children with a Rare Disease at Diagnosis (No. 00001). RBW Consulting were not involved in the design, performance, analysis or interpretation of this research, or writing of the manuscript.
Conflicts of interest
All authors declared that there are no conflicts of interest.
Ethical approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Copyright
© The Author(s) 2022.
REFERENCES
1. Anderson M, Elliott EJ, Zurynski YA. Australian families living with rare disease: experiences of diagnosis, health services use and needs for psychosocial support. Orphanet J Rare Dis 2013;8:22.
2. Kole A, Faurisson F. The voice of 12,000 patients: experiences and expectations of rare disease patients on diagnosis and care in Europe; Paris, France: EURORDIS - Rare Diseases Europe, 2009.
3. Grigull L, Mehmecke S, Rother AK, et al. Common pre-diagnostic features in individuals with different rare diseases represent a key for diagnostic support with computerized pattern recognition? PLoS One 2019;14:e0222637.
4. Zurynski Y, Deverell M, Dalkeith T, et al. Australian children living with rare diseases: experiences of diagnosis and perceived consequences of diagnostic delays. Orphanet Journal of Rare Diseases 2017;12:68. 10.1186/s13023-017-0622-4.
5. Blöß S, Klemann C, Rother AK, et al. Diagnostic needs for rare diseases and shared prediagnostic phenomena: Results of a German-wide expert Delphi survey. PLoS One 2017;12:e0172532.
6. Germeni E, Vallini I, Bianchetti MG, Schulz PJ. Reconstructing normality following the diagnosis of a childhood chronic disease: does “rare” make a difference? Eur J Pediatr 2018;177:489-95.
7. Houdayer F, Gargiulo M, Frischmann M, et al. The psychological impact of cryptic chromosomal abnormalities diagnosis announcement. Eur J Med Genet 2013;56:585-90.
8. Pelentsov LJ, Laws TA, Esterman AJ. The supportive care needs of parents caring for a child with a rare disease: A scoping review. Disabil Health J 2015;8:475-91.
9. Liberati A, Altman DG, Tetzlaff J, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ 2009;339:b2700.
10. Moher D, Liberati A, Tetzlaff J, Altman DG. PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 2009;21:e1000097.
11. Atasoy R, Sevim C. Evaluation of coping strategies with stress of parents who have mentally disabled children in northern Cyprus. Universal Journal of Educational Research 2018;6:1129-40.
12. Berrocoso S, Amayra I, Lázaro E, et al. Coping with wolf-Hirschhorn syndrome: quality of life and psychosocial features of family carers. Orphanet J Rare Dis 2020;15:293.
13. Boettcher J, Denecke J, Barkmann C, Wiegand-Grefe S. Quality of life and mental health in mothers and fathers caring for children and adolescents with rare diseases requiring long-term mechanical ventilation. Int J Environ Res Public Health 2020;17:8975.
14. Dellenmark-Blom M, Chaplin JE, Jönsson L, et al. Coping strategies used by children and adolescents born with esophageal atresia - a focus group study obtaining the child and parent perspective. Child Care Health Dev 2016;42:759-67.
15. Dellve L, Samuelsson L, Tallborn A, Fasth A, Hallberg LR. Stress and well-being among parents of children with rare diseases: a prospective intervention study. J Adv Nurs 2006;53:392-402.
16. Douma M, Bouman CP, van Oers HA, et al. Matching psychosocial support needs of parents of a child with a chronic illness to a feasible intervention. Matern Child Health J 2020;24:1238-47.
17. Glenn AD. Using online health communication to manage chronic sorrow: mothers of children with rare diseases speak. J Pediatr Nurs 2015;30:17-24.
18. Hilliard ME, Tully C, Monaghan M, Wang J, Streisand R. Design and development of a stepped-care behavioral intervention to support parents of young children newly diagnosed with type 1 diabetes. Contemp Clin Trials 2017;62:1-10.
19. Kountz-Edwards S, Aoki C, Gannon C, et al. The family impact of caring for a child with juvenile dermatomyositis. Chronic Illn 2017;13:262-74.
20. Krabbenborg L, Vissers LE, Schieving J, et al. Understanding the psychosocial effects of wes test results on parents of children with rare diseases. J Genet Couns 2016;25:1207-14.
21. Lakshmanan A, Kubicek K, Williams R, et al. Viewpoints from families for improving transition from NICU-to-home for infants with medical complexity at a safety net hospital: a qualitative study. BMC Pediatr 2019;19:223.
22. Lauder B, Sinclair PM, Maguire J. Mothers’ experience of caring for a child with early onset scoliosis: A qualitative descriptive study. J Clin Nurs 2018;27:e1549-60.
23. Merker VL, Plotkin SR, Charns MP, et al. Effective provider-patient communication of a rare disease diagnosis: A qualitative study of people diagnosed with schwannomatosis. Patient Educ Couns 2021;104:808-14.
24. Pelentsov LJ, Fielder AL, Laws TA, Esterman AJ. The supportive care needs of parents with a child with a rare disease: results of an online survey. BMC Fam Pract 2016;17:88.
25. Picci RL, Oliva F, Trivelli F, et al. Emotional burden and coping strategies of parents of children with rare diseases. J Child Fam Stud 2015;24:514-22.
26. Rice DB, Carboni-Jiménez A, Cañedo-Ayala M, et al. Perceived benefits and facilitators and barriers to providing psychosocial interventions for informal caregivers of people with rare diseases: a scoping review. Patient 2020;13:471-519.
27. Senger BA, Ward LD, Barbosa-Leiker C, Bindler RC. Stress and coping of parents caring for a child with mitochondrial disease. Appl Nurs Res 2016;29:195-201.
28. Shapiro E, Lourenço CM, Mungan NO, et al. Analysis of the caregiver burden associated with Sanfilippo syndrome type B: panel recommendations based on qualitative and quantitative data. Orphanet J Rare Dis 2019;14:168.
29. Siddiq S, Wilson BJ, Graham ID, et al. Experiences of caregivers of children with inherited metabolic diseases: a qualitative study. Orphanet J Rare Dis 2016;11:168.
30. Silibello G, Vizziello P, Gallucci M, et al. Daily life changes and adaptations investigated in 154 families with a child suffering from a rare disability at a public centre for rare diseases in Northern Italy. Ital J Pediatr 2016;42:76.
31. Simpson A, Ross R, Porter J, et al. Adrenal insufficiency in young children: a mixed methods study of parents’ experiences. J Genet Couns 2018;27:1447-58.
32. Somanadhan S, Larkin PJ. Parents’ experiences of living with, and caring for children, adolescents and young adults with Mucopolysaccharidosis (MPS). Orphanet J Rare Dis 2016;11:138.
33. Toledano-Toledano F, Luna D. The psychosocial profile of family caregivers of children with chronic diseases: a cross-sectional study. Biopsychosoc Med 2020;14:29.
34. van de Loo KFE, Custers JAE, Koene S, et al. Psychological functioning in children suspected for mitochondrial disease: the need for care. Orphanet J Rare Dis 2020;15:76.
35. van der Kloot WA, Hamdy NAT, Hafkemeijer LCS, et al. The psychological burden of an initially unexplained illness: patients with sternocostoclavicular hyperostosis before and after delayed diagnosis. Health Qual Life Outcomes 2010;8:97.
36. Witt S, Dellenmark-Blom M, Dingemann J, et al. Quality of life in parents of children born with esophageal atresia. Eur J Pediatr Surg 2019;29:371-7.
37. Wu YH, Sun FK, Lee PY. Family caregivers’ lived experiences of caring for epidermolysis bullosa patients: a phenomenological study. J Clin Nurs 2020;29:1552-60.
38. Yamaguchi K, Wakimizu R, Kubota M. Difficulties in daily life and associated factors, and QoL of children with inherited metabolic disease and their parents in Japan: a literature review. JIMD Rep 2017;33:1-10.
39. Zengin M, Yayan EH, Akıncı A. Difficulties experienced by Turkish parents and their coping strategies: children with mucopolysaccharidosis. J Pediatr Nurs 2020;53:e142-8.
40. McConkie-Rosell A, Hooper SR, Pena LDM, et al. ; Undiagnosed diseases network. Psychosocial profiles of parents of children with undiagnosed diseases: managing well or just managing? J Genet Couns 2018;27:935-46.
41. Heuyer T, Pavan S, Vicard C. The health and life path of rare disease patients: results of the 2015 French barometer. Patient Relat Outcome Meas 2017;8:97-110.
42. Llubes-Arrià L, Sanromà-Ortíz M, Torné-Ruiz A, et al. Emotional experience of the diagnostic process of a rare disease and the perception of support systems: A scoping review. J Clin Nurs 2022;31:20-31.
43. Depping MK, Uhlenbusch N, von Kodolitsch Y, et al. Supportive care needs of patients with rare chronic diseases: multi-method, cross-sectional study. Orphanet J Rare Dis 2021;16:44.
44. McMullan J, Crowe AL, Bailie C, et al. Improvements needed to support people living and working with a rare disease in Northern Ireland: current rare disease support perceived as inadequate. Orphanet J Rare Dis 2020;15:315.
45. Waldron R, Hall K. Psychosocial support for families following a child’s diagnosis of type 1 diabetes. Diabetes Care for Children & Young People 2020;9.
46. Masulani-Mwale C, Kauye F, Gladstone M, Mathanga D. Development of a psycho-social intervention for reducing psychological distress among parents of children with intellectual disabilities in Malawi. PLoS One 2019;14:e0210855.
47. Martin K, Geuens S, Asche JK, et al. Psychosocial recommendations for the care of children and adults with epidermolysis bullosa and their family: evidence based guidelines. Orphanet J Rare Dis 2019;14:133.
48. Kaplan M. SPIKES: a framework for breaking bad news to patients with cancer. Clin J Oncol Nurs 2010;14:514-6.
49. Ahanotu CJ, Ibikunle Po, Hammed AI. Burden of caregiving, social support and quality of life of informal caregivers of patients with cerebral palsy. Turkish Journal of Kinesiology 2018;4:58-64.
50. Bogart KR, Frandrup E, Locke T, et al. “Rare place where I feel normal”: Perceptions of a social support conference among parents of and people with Moebius syndrome. Res Dev Disabil 2017;64:143-51.
51. Bogart KR, Hemmesch AR. Benefits of support conferences for parents of and people with Moebius syndrome. Stigma and Health 2016;1:109-21.
52. Haukeland YB, Fjermestad KW, Mossige S, Vatne TM. Emotional experiences among siblings of children with rare disorders. J Pediatr Psychol 2015;40:712-20.
53. NHS. European reference centres networks. Available from: https://www.england.nhs.uk/publication/uk-endorsed-ern-centres/ [Last accessed on 31 Mar 2022].
54. Smith M, Alexander E, Marcinkute R, et al. Telemedicine strategy of the European Reference Network ITHACA for the diagnosis and management of patients with rare developmental disorders. Orphanet J Rare Dis 2020;15:103.
55. Global Commission. Ending the diagnostic odyssey for children with a rare disease year one report. Available from: https://www.globalrarediseasecommission.com/Report [Last accessed on 31 Mar 2022].
56. Global Commission. Ending the diagnostic odyssey for children with a rare disease. Available from: https://www.globalrarediseasecommission.com/OurWork [Last accessed on 31 Mar 2022].
57. NHS. Highly specialised services. Available from: https://www.england.nhs.uk/commissioning/spec-services/highly-spec-services/ [Last accessed on 31 Mar 2022].
58. BBS UK. Overview of BBS clinics service. Available from: https://bbsuk.org.uk/bbs-clinics-overview/ Last accessed on 31 Mar 2022].
59. Department of Health & Social Care. The UK rare diseases framework. Available from: https://www.gov.uk/government/publications/uk-rare-diseases-framework [Last accessed on 31 Mar 2022].
Cite This Article
Export citation file: BibTeX | RIS
OAE Style
Kenny T, Bogart K, Freedman A, Garthwaite C, Henley SMD, Bolz-Johnson M, Mohammed S, Walton J, Winter K, Woodman D. The importance of psychological support for parents and caregivers of children with a rare disease at diagnosis. Rare Dis Orphan Drugs J 2022;1:7. http://dx.doi.org/10.20517/rdodj.2022.04
AMA Style
Kenny T, Bogart K, Freedman A, Garthwaite C, Henley SMD, Bolz-Johnson M, Mohammed S, Walton J, Winter K, Woodman D. The importance of psychological support for parents and caregivers of children with a rare disease at diagnosis. Rare Disease and Orphan Drugs Journal. 2022; 1(2): 7. http://dx.doi.org/10.20517/rdodj.2022.04
Chicago/Turabian Style
Kenny, Thomas, Kathleen Bogart, Albert Freedman, Claire Garthwaite, Susie M. D. Henley, Matt Bolz-Johnson, Shehla Mohammed, Jill Walton, Kym Winter, Deborah Woodman. 2022. "The importance of psychological support for parents and caregivers of children with a rare disease at diagnosis" Rare Disease and Orphan Drugs Journal. 1, no.2: 7. http://dx.doi.org/10.20517/rdodj.2022.04
ACS Style
Kenny, T.; Bogart K.; Freedman A.; Garthwaite C.; Henley SMD.; Bolz-Johnson M.; Mohammed S.; Walton J.; Winter K.; Woodman D. The importance of psychological support for parents and caregivers of children with a rare disease at diagnosis. Rare. Dis. Orphan. Drugs. J. 2022, 1, 7. http://dx.doi.org/10.20517/rdodj.2022.04
About This Article
Copyright
Data & Comments
Data
 Cite This Article 64 clicks
Cite This Article 64 clicks












Comments
Comments must be written in English. Spam, offensive content, impersonation, and private information will not be permitted. If any comment is reported and identified as inappropriate content by OAE staff, the comment will be removed without notice. If you have any queries or need any help, please contact us at support@oaepublish.com.